BOSTON, May 6, 2021 /PRNewswire/ -- Use of outpatient mental health services, including psychotherapy, increased nearly 20% during the COVID-19 crisis, and spending on substance use disorder treatment increased by 10%, according to data released today by Blue Cross Blue Shield of Massachusetts ("Blue Cross"). Nearly three quarters of members' mental health visits during the pandemic have been conducted via telehealth, either via phone or virtually, and 60% of mental health diagnoses made via telehealth have been for anxiety.
March 2020-March 2021 | |
Number of telehealth visits (both physical and mental health) | 8 million |
Increase in telehealth visits over prior year | 9,500% |
Percentage of telehealth visits focused on mental health | 54% |
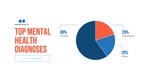
Top mental health diagnoses via telehealth | Anxiety (60%) |
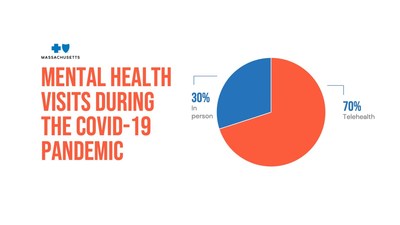
Percentage of outpatient mental health visits conducted via telehealth vs. in person | 70% |
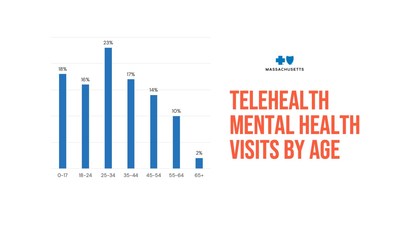
Demographics of members using telehealth for mental health services | 18% ages 0-17 |
Members enrolling in Learn to Live digital platform for anxiety, depression, insomnia & stress | 1,000 per month |
"Unlike medical services, which were largely deferred during the first several months of the pandemic, mental health claims have increased significantly," said Dr. Ken Duckworth, senior medical director for behavioral health at Blue Cross. "Kids, teens, adults – we're seeing unprecedented demand for care. The good news is that our members are getting help – both in-person and virtually."
Mental health care via telehealth
Members' telehealth use has skyrocketed since Blue Cross expanded coverage for telephone and virtual visits during the COVID-19 crisis. The company has processed more than 8 million telehealth claims since the start of the pandemic, 54% of which have been for mental health care. Blue Cross' spending on telehealth is more than 100 times what it was in 2019, and the number of telehealth visits increased by 9,500% in 2020.
"This has been a transformation in care delivery unlike anything I've ever seen," noted Dr. Duckworth. "We're going to see sustained interest in telehealth for mental health care, even after the pandemic subsides. Many members tell us they appreciate the convenience and added flexibility virtual care offers, and clinicians report fewer missed or cancelled appointments. While there are obviously some exceptions, the feedback we've heard from patients and practitioners has been largely positive."
Substance use disorder
While other types of care – including elective surgery and preventive screenings - declined significantly during the early months of the pandemic, claims for substance use disorder (SUD) care dipped only slightly, and Blue Cross' spending on these services increased by 10%. Members who received SUD care prior to the COVID crisis used more of those services during the public health emergency.
"The entire addiction treatment field was disrupted almost overnight," said Dr. Gregory Harris, senior medical director for behavioral health at Blue Cross. "The pandemic affected every aspect of substance use disorder care, but fortunately, we were able to work with clinicians to find creative solutions. Telehealth allowed many members to continue to get the SUD treatment they needed, even for higher levels of care like intensive outpatient and partial hospitalization programs."
Blue Cross took several steps to improve members' access to SUD services via telehealth during the pandemic, including allowing visits to be conducted via both video and phone, since telephonic visits may be particularly useful for members who do not have internet access or privacy.
More members using online tools to improve mental health
The number of members using digital platforms to manage their mental health has increased rapidly since the pandemic began. In July 2020, BCBSMA launched Learn to Live to its fully insured customers and members at no additional cost to improve access to mental health resources during the COVID crisis. Learn to Live provides self-guided, interactive digital programs to help members with stress, anxiety, depression, and substance use conditions.
Participation has exceeded expectations with more than 1,000 members per month enrolling in the program. 60% of these members had not previously been in therapy for these conditions. Blue Cross members using Learn to Live to address depression or stress, anxiety and worry report an average improvement of 30%.
Connecting members with the right care
To help meet the unprecedented demand for emotional support during the pandemic, Blue Cross has added more than 500 new mental health clinicians to its network since March 2020 via its expedited emergency credentialing and enrollment process. This brings the total number of psychologists, psychiatrists, social workers, family therapists and other mental health clinicians in the Blue Cross network – most of whom are now offering telehealth services - to nearly 15,000. This comes on the heels of Blue Cross' announcement of bold new initiatives to ensure members have timely access to high-quality, affordable mental health care and substance use disorder.
Blue Cross members who need assistance finding mental health and/or substance use disorder services can visit the company's mental health resource center or call the number on their member ID card. Blue Cross representatives can help locate appropriate clinicians who are accepting new patients and even assist with setting up the first visit.
About Blue Cross Blue Shield of Massachusetts
Blue Cross Blue Shield of Massachusetts (www.bluecrossma.org) is a community-focused, tax-paying, not-for-profit health plan headquartered in Boston. We are committed to the relentless pursuit of quality, affordable health care with an unparalleled consumer experience. Consistent with our promise to always put our members first, we are rated among the nation's best health plans for member satisfaction and quality. Connect with us on Facebook, Twitter, YouTube, and LinkedIn.
- BlueLinks for Employers
- BlueLinks for Providers
- BlueLinks for Brokers
- Get Blue MA
- Blue Cross Foundation
SOURCE Blue Cross Blue Shield of Massachusetts